Dr Rajat Goel
is India's leading
Bariatric Surgeon
and Allurion Balloon Specialist.
Why patients choose
Dr Rajat Goel
15000+
Laparoscopic Surgeries
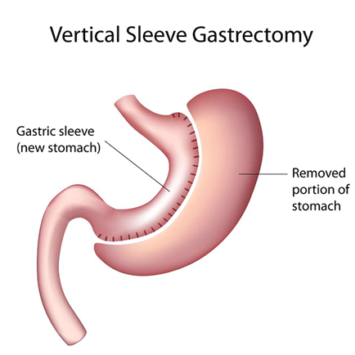
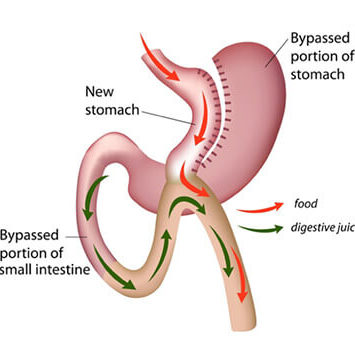
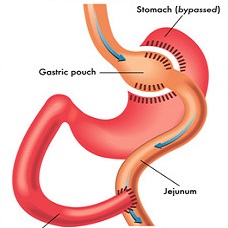
1500+
Bariatric Surgeries
1000+
Laser Surgeries
100+
Allurion Balloon
21+
Years of experience
42+
Countries

Dr Rajat Goel —
A Leading Minimal Access Robotic and Laser Surgeon
Dr. Rajat Goel is a trained Minimal Access and Bariatric surgeon having done his MBBS from prestigious Maulana Azad Medical College, and MS (Master of Surgery) from Lady Hardinge Medical College with advanced laparoscopic training at Taiwan, Singapore, and USA.
21+ years of experience
Meet our team
Featured Videos
Allurion Balloon Procedure For Weight Loss
Laser Piles or Hemorrhoids Surgery
What is Obesity? | Why Obesity is Dangerous?
Patient Testimonials about Allurion Balloon for Weight Loss
Frequently Asked Questions!
What Can You Eat After Bariatric Surgery?
Post Bariatic Surgery Dieting Phases
Why You Shouldn’t Fear Bariatric Surgery?
Post Bariatric Surgery Excercise – 1
What Exercises We Do After Bariatric Surgery?
Post Bariatric Surgery Excercise – 2